percy pippin | a birth story
When I was 20 weeks pregnant I asked my midwife if the rumours were true: “Are third births generally unpredictable?” She turned away from the computer, looked me in the eye and with every ounce of her knowing, replied: “Every birth is unpredictable.”
………………………………………………………………………………………
The last few weeks of my pregnancy were hot and sticky; the humidity was stifling and I had taken to crunching cup loads of ice to maintain some semblance of cool. I swam in the ocean most days, grateful for the buoyancy, and did my best to mentally prepare for what lay ahead.
I was 39+1 weeks when I felt the distinct shift. It was a Sunday in early March and I was crying whilst doing the dishes. I didn’t want to see anyone or go anywhere and the braxton hicks had become mild yet persistent contractions. I had arrived at that uncomfortable, challenging, emotional place they call “the in-between”. My patience ebbed and flowed for the days that followed as I walked and squatted and danced and rested.
On Thursday morning I had an acupuncture treatment. It was my third in as many weeks and my acupuncturist confirmed what I already knew; my body was ready, I just had to wait for my baby. Later that afternoon, on the way to the hospital to see my midwife, Val, the contractions grew stronger and more frequent and whilst I didn’t want to get attached to the possibility that this might be it, there was a big part of me that willed it to be so.
I went to bed that night and woke the next morning – no progression, still pregnant. I got up and made Che’s school lunch and carried on with the day. But as I did the washing and made the beds there was a little inkling that demanded my attention. Something wasn’t quite right and it began to unsettle me – a mother’s intuition.
Saturday marked my due date according to my calendar so I took myself off for a pedicure and encouraged the beautician to firmly massage my feet, focussing on the acupressure points that encourage labour to start. That afternoon I continued to sway and swim and squat, rubbing my belly downwards to encourage baby’s head to press on the cervix. My beloved midwife was officially on annual leave but she wanted to stay on call all weekend so she could be with me if I went into labour. It was with much relief that I woke at 12:45am on Sunday morning to find that my waters had broken.
We were at the hospital by 2am and whilst I was having contractions they weren’t strong or productive. The midwife on duty went through the necessary steps post waters breaking, including half-an-hour of monitoring to ensure baby’s heart-rate was normal. I was fine, baby was fine, but labour wasn’t progressing. As I suspected, she recommended I go home and rest and wait for the contractions to start. If they hadn’t by 7am on Monday, I would have to go to the main hospital for induction.
I make pancakes and, more importantly, get labour going. I was exhausted and scared yet determined to come back to the idea of letting go and, ultimately, surrendering. I felt like my baby had been patient with me throughout the pregnancy and now it was my turn to repay the favour.
As I poured pancake batter into the frying pan I started thinking about acceptance. Time and time again I had talked to my pre-natal students about accepting where the birth journey takes you; because often it is completely beyond your control. I gave myself a talking to then and whilst the idea of an assisted birth or cesarean had always petrified me, I began to prepare myself for the possibility of a birth so wildly different from my past experiences.
Val visited me mid-afternoon and massaged my feet and legs, applying pressure to those points that naturally induce labour. I was contracting while she was with me and she encouraged me to squat deeply in each contraction to encourage the head to move down. Once she left I began packing a bag for Che and Poet to take to my parent’s house. By 4:30pm Daniel and I were home alone so we walked the beach and I continued to squat and sway and walk and wait.
By 7pm I was in bed, resting and trying to relax. The contractions were becoming more frequent and starting to require all of my awareness so it was with much gratitude that we drove to the hospital at 9pm. Once there, the contractions slowed and weakened, and whilst Daniel was happy to rub my back and feed me ice-cubes, I encouraged him to get some sleep. Disheartened, I knew that I needed some time alone to walk the wards.
A wooden handrail conveniently featured on every wall of the maternity ward so I held onto it in each contraction and moved into a deep squat whilst exhaling. Val soon joined me and we talked about what was happening, or more precisely, what wasn’t happening. “I just don’t understand why this baby isn’t moving down,” I said. It was shortly after midnight when I gave in and told her I was going to rest. She agreed that it was the best thing to do.
At 3am we surrendered to the fact that labour wasn’t going to happen on its own so we drove to the main hospital to commence induction. I sobbed in the car, so full of fear and worry for the safety of my baby. Regardless of the strong heartbeat that I heard every time the doppler was placed on my belly, I knew that there was something not quite right.
The hours that followed were painful and tiring – I had only slept for five hours in the past two days. The canula pumped syntocin into my system and slowly, slowly, I started having strong, productive contractions. I had two wireless monitors on my belly – one to monitor baby’s heartbeat and the other to monitor the contractions – and I watched the numbers on the screen beside me. By 6am we began to notice baby’s heartbeat dropping with each contraction but as soon as the contraction eased, the heartbeat recovered nicely. Val mentioned “cord compression” and whilst the midwives were keeping an eye on the numbers, they weren’t overly concerned.
By 7:30am Val said goodbye – she had been with us all night and needed to rest. As she left the room, baby’s heartbeat soon dropped and didn’t recover for two contractions. One of the midwives conveniently moved the screen so I could no longer see the numbers but as my contractions were getting more intense, there was a growing sense of unease amongst those supporting me.
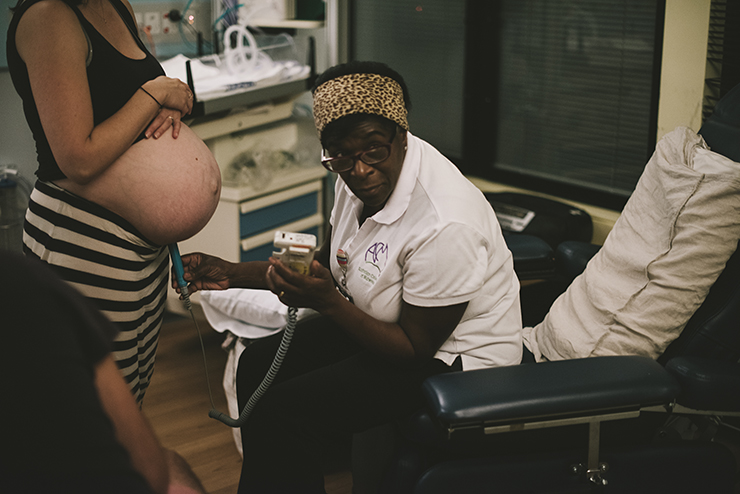
I was lying on my side at this stage and felt the urge to push. Every single cell in my body wanted to push but when Kate, the obstetrician, checked me, she told me I couldn’t – I was only 6cm and had a cervical lip. It was the most challenging place I had ever been – trying not to push when that’s all my body wanted to do and attempting to breathe through the most painful contractions I had ever experienced. I did what I had taught hundreds of my students to do; I lifted my chin to relieve the pressure in my pelvis and I breathed short, sharp exhalations out of my mouth, focussing my gaze directly into Daniel’s eyes.
The events that followed are a blur, but they go something like this:
After a monitor had been placed on baby’s head to get a more accurate reading of his heartbeat, Kate told me that they were going to take a sample of his blood to read his lactic acid levels. We all knew that he was distressed and I knew, with all my being, that he needed to be born – quickly. Any fear I once harboured about a caesarean birth soon dissipated and I fell into the most vulnerable place I have ever been. I was rocking on the bed, breathing through a contraction, while one midwife took off my clothes and dressed me in a hospital gown, another covered my jewellery in tape, Daniel reassured and encouraged me and Kate attempted to move the cervical lip. They were preparing me for a cesarean but Kate wanted to attempt a vaginal delivery first. If successful, it was going to be much quicker than the alternative.
I said out loud: “I’m so scared for my baby, I just want my baby” – the fear coupled with the pain was overwhelming and yet there was also an element of calm; I knew that the best thing I could do was breathe deep and listen to the OB, so I did. Kate looked me in the eye at this stage and took me through what we needed to do to get baby out. My legs were in stirrups and she placed the vacuum on his head and for the next contraction I pushed with all my might. His head was born and we finally knew why he resisted moving into the pelvis: “Cord around the neck once, twice, three times”. Minutes later he was born and placed on my chest; he was blue but then he cried and I exhaled. He was here and he was safe.
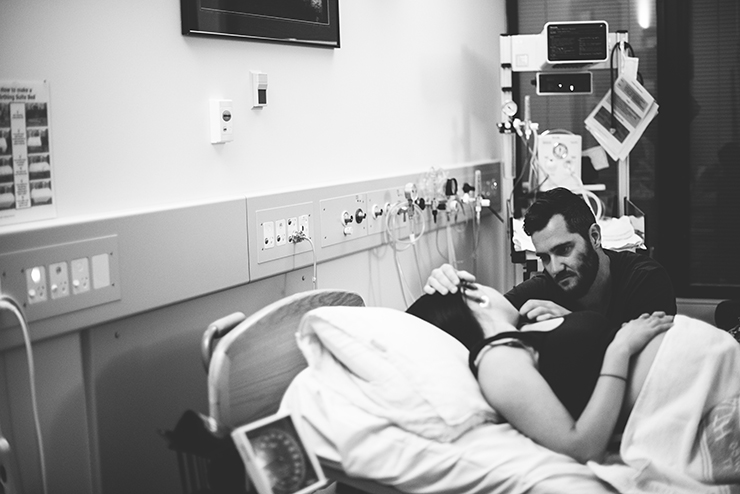
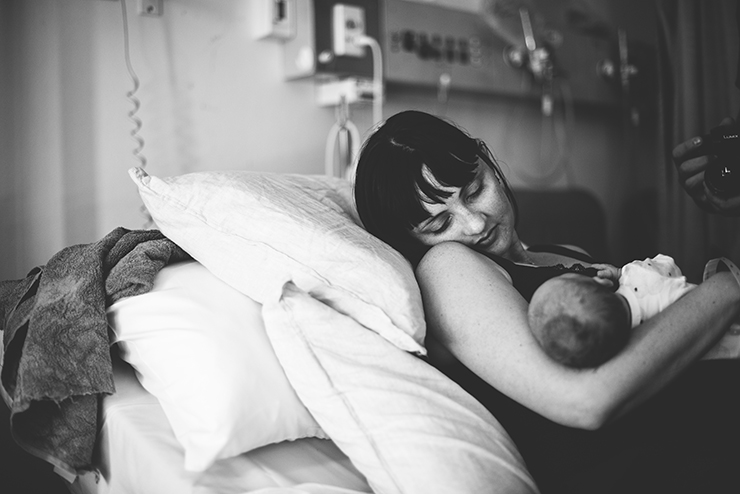
He stayed on my chest for half-an-hour and I smelt him, kissed him, calmed him. He was quite stressed after the birth and his breathing was shallow and fast so the Paediatrician took him to Special Care to be monitored and Daniel followed, camera in hand.
I stayed behind, drank tea and cried.Every midwife, doctor and specialist that was present in the room during delivery was a stranger to Daniel and I. And yet individually and collectively they expressed a deep sense of respect to me as the birthing mother and to Daniel as the supportive, yet concerned, partner. Perhaps it was just another day in birthing suite for them but I’ll always be thankful for what they did for us. I’ll always remember the kind words that were spoken and, more distinctly, the gentle way I was touched and held during the delivery.
When Daniel returned from Special Care he got me into the shower and stood beside me as I let the water fall onto my lower back. I was sore and exhausted and the canula rendered my right hand unusable so, once I was clean, he wrapped me in a towel, walked me towards the bed and dressed me. And then he held my hand and walked me down to the nursery and together we sat beside Percy’s cot and gazed at him; proud, relieved parents falling deeply in love – with each other and our newborn son.
Percy’s birth was nothing like I envisioned yet it was no less beautiful than I expected.

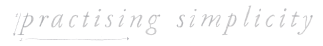












Thank you for sharing your story of Percy's birth. As a student midwife I provide continuity of care to women (in a student capacity) and I have just finished being 'on-call' for 5 women this month, two of which had very similar experiences to yours. The strength of mind and body of women in these circumstances continues to amaze me and so too does that of the staff that care for them. Thanks again for reiterating that a complex birth has much to teach and be marvelled over.
Thank you for sharing such a deeply personal journey, Jodi. It was a blessing to read this.
Every birth is unpredictable and every birth is beautiful. Thank you for sharing Percy's, Jodi. x
Such a beautiful story – it's so lovely to write these things down because it's wonderful to be able to remember these things as our memories fade over time.
So beautiful. Thank you for sharing.
Made me teary.
Percy is perfect.
What a lovely post. Thank you for sharing. My first baby was a very difficult birth. She was also in distress. There were about 8 people in the room, but they supported me in trying to have a vaginal birth (which I did) and kept our mind off darker thoughts by guessing the sex, commenting on her hair, smiling calmly. It was such a wonderful, positive birth and like you, I will forever feel love for those that helped me meet my daughter.
What a beautiful, moving birth story and so wonderful to hear that even when intervention was needed it was done in a respectful and caring way, just beautiful photos too, so much love, thanks for sharing.
Very glad he was delivered safely and with the cord wrapped around his neck three times that is very scary.
Thank you for sharing your birth story with us. Amazing, really. You are so strong and should be so proud. In the US women aren't allowed to have more than 12 or 14 hours or something after their water breaks. They gave you the time and freedom to get that baby out. Go get your push present now. 🙂
I am 6 days post labour today and this made me cry my eyes out. Both my births have resulted in emergency c-sections despite my desperate attempts to deliver vaginally. In their own way my children have taught me that control
Is not everything, but it has been an extremely difficult lesson to recognise and comprehend. Thank you for sharing your story so honestly x
So sweet Jodi! It brought tears to my eyes reading your story. It brought me back to all the emotions I had with the days leading up to my labor, during the labor and afterwards! Labor is such a wild and scary ride with no real control. Many happy blessings again to your family and newest addition! -Lissa
I can't believe you went through all of that without pain relief, wow! Percy's lucky to have such a strong and determined mum.
p.s. I've always been amazed at how wildly different a woman's pregnancy and birth experiences can be, from one baby to the next. Birth is, as you said, unpredictable. x
I'm sitting here with tears in my eyes.
What a journey labor is for all of us, l too am reliving all the emotions l felt with the birth of my daughter (24 hour labor that ended in an emergency cesarean…the term "failure to progress" still rings in my ear).
Thank you for sharing such a personal experience Jodi, l do believe that great things can be achieved with such honesty. And for the first time ever, l'm motivated to put what l remember about my daughters birth (seven years ago) down on paper.
So emotional and beautiful jodi, tears are streaming. I'm glad he was delivered safe and healthy, precious Percy. xo
Sp happy for you, and what a beautiful story! Love his handsome name, too. Congratulations!
http://beccagarber.com/why-have-friends-over-for-dinner/
beautiful jodi, so emotional and so courageous. It took me right back to Olive's birth story. My birth plans were always to just go with whatever my baby and my body dictated, as challenging and frightening as it may be. But then when you realise something is not quite right, surrendering to the situation at hand and birthing your baby safely is all that matters in the end..love to you all x
Thankyou for sharing your story, or you and Percy's journey really…midwives are a special breed aren't they. I had a known and trusted midwife for my first two babies, which was so reassuring. For my third, I was apprehensive about not knowing my midwife. I met her an hour before he was born but I felt no less supported and reassured during the birth, for which I am so grateful.
I really have no words. Pure and simple and beautiful. Congratulations xx
I had a lump in my throat reading this Jodi. I'm so pleased Percy arrived in good health and you and him were safe and are together at last xx
What a blessing that Percy arrived safely, and all is well! Beautiful, touching photos of a special time.
So touching. A beautiful journey.
Every birth story, regardless of the challenges is beautiful. Thank you for sharing. I just love the tenderness and care your husband showed to you, post birth, as you described. Love could be shown in no greater way at that time.
So glad he is here and safe. This is a beautiful story.
Beautiful, brought me to tears. Thank you for sharing
Thanking God that you are both safe.
Love,
Ronnie xo
What a beautiful family you are. I had a similar experience at home – not not so many days, though, and my waters didn't break til the end. But yes, my daughter never really dropped until the end of labour and her heart rate was fine throughout. I was at home with an independent midwife and she was confident of the strong heart beat, so we waited it out.
My midwife felt that she'd stayed high so long because of the cord, and then come out very fast in the end as a way of keeping herself safe.
I'm pretty sure if I'd gone to hospital here in Ireland, I would have been induced, and the contraction stress you describe would have led to a section very fast. I'm glad you didn't have to go that far!
Your son is gorgeous, and his name is so perfect, I love it. I'm so happy that things worked out well.
Also, has he been to a cranio sacral osteopath for babies? It would help soothe and correct the effects of the cord and the induction contractions and the ventouse very well.
Best wishes! Jo x
A lovely read! There's nothing quite like welcoming a beautiful new baby. I could keep having babies forever!
Congratulations! Healthy baby, healthy mumma, that's what matters. My two boys were born by Caesarian. I didn't want one at either time, but they were what I needed to have for baby's and my health. Take care and thanks for sharing. xxoo
Oh Jodi I am so relieved for you and your little family at Percy's safe arrival. At 31 weeks pregnant I am up early this morning and have just read this story through the tears at my craft table with a bowl of cereal. It has really struck me. I know I will find strength when I need it to birth my baby but the worry and unpredictability of it all is just so scary. The poor little guy with the cord around his neck. I mean! Thank you for sharing this beautiful story xxx Jen
So happy he is safe and surrounded by pure love. Thank you for sharing
So glad you and Percy Pippen are safe and well! He is a beautiful baby. Thank you for sharing your story. And the photos are amazing. The one of the moment with you and Daniel before the delivery just speaks so much. Congratulations again, Jodi!
Ah births. They're nuts. I had a very similar experience with my first – days of labour pains that never went anywhere, an induction when I was already tired and disheartened, a stuck and distressed baby, and a (for me, very traumatic) ventouse. It taught me that you can do everything right, be in the right head space, try hard and trust yourself, and can still have something other than a peaceful, natural birth. I'm so glad you felt supported, it makes all the difference. Such a beautiful mama 🙂
Thank you for sharing your story with us Jodi. I'm in the process of writing about Alby's birth – something that always seems to take me a very long time, such is the sacredness of the event, perhaps. I'm so glad, that despite being so different to that of your first two, your experience was no less beautiful – a true testament to you as a mother and person xxx
Beautiful. x
Oh Jodi, this is such a special story – I read it having birthed my baby boy just four days ago. He is my second and his birth was so different in its own way from my first but just as potent and precious. Bless you and your little Percy xx
Thank you for sharing this story. I'm 32 weeks pregnant with number 2 and trying to get my head around birthing this baby as first birth was a rapid emergency c-section due to placental abruption at 38 weeks. So there's some fears about it all. So many birth stories on the Internet seem to be from women with strong feelings about a particular way of birthing. It has been very comforting to read your story of a hospital birth that had difficulties but was beautiful and respectful. I suspect I will be returning to read this again in the next few weeks. Congratulations and thanks
Absolutely beautiful, how unpredictable birth is but just what new life is. x
I really appreciated reading your story. I am expecting my third baby in June and have had similar thoughts and feelings about what a 3rd labor will be like, interventions and c-sections, etc as you seem to have had. I found your story comforting and reassuring. Knowing that we have to surrender to the process and give up our sense of control has been a lesson for me each of the other two times, and I can tell it's going to be that way this time too. I am so glad your care providers at the hospital were respectful and gentle and that you see the absolute beauty in Percy's birth. I had a hospital birth with my first and a birth center birth with my second – very different experiences, but both beautiful. I keep wondering in which way birth #3 will be different. 🙂
I read these words and cried, I had Squawk in that same hospital, and when everything was going pear shaped I remember just reminding myself to surrender. Your story, his story is lovely. Congratulations.
What a beautiful story and a beautiful, sweet baby. Thank you for sharing.
I suddenly realised I hadn't read your birth story yet Jodes – this was beautiful. Makes me love Daniel. Congratulations to you both (parents of three! Eek!) xxx
So beautifully told, Jodie. I had a third birth experience that was completely different from the previous two (actually they were all quite different!), and I narrowly avoided an emergency caesarean with the help of some amazing midwives (my baby was transverse but nobody realised this until several hours in the hospital). I was quite traumatised by the experience and it took me a long time to be able to talk about my experience without bursting into tears. I love the final line of your story – I can now, 3 years later, see that my own experience was also a beautiful one. xx
wow. logging in after a big absence, i was so moved to read this jodi. and so so relieved to hear that it all went well. thankyou for sharing and blessings on the growth and evolution of your family and personal journey as a mama of 3! Blessings. Tali